Editorial by Matt Palaszynski, Founder BRIGHT Foundation
Using my family’s personal journey of a global search for brain injury treatments over the last 25 years, I would like to highlight one of the most under-discussed realities in neurorehabilitation: The contrast between the acute phase revolution and the chronic phase stagnation. Hopefully, my personal story will help frame a powerful—and heartbreakingly accurate discussion illustrating that long term brain injury recovery remains a landscape of incrementalism, and unrealized hope.
This article is not intended to discourage families newly navigating a Cerebral Palsy diagnosis, nor to criticize the dedicated professionals and researchers working in the field. Instead, it serves as a wake-up call: breakthroughs in brain injury treatment are possible—and history proves they happen. With rapid advances in computational power, artificial intelligence, and our fundamental understanding of brain function, we are approaching a tipping point that could unlock the next major leap forward. This article is a call to action—for bold innovation, increased funding, and meaningful policy reform.
The Two Worlds of Brain Injury Treatment
At the highest level, this article explores a stark divide: we can summarize by saying that brain injury treatment in the first 72 hours of life has seen dramatic advances, but treatment beyond that window has remained largely stagnant for the past 25 years.
| Phase | Timeframe | Progress | Key Treatment | Outcome Impact |
|---|---|---|---|---|
| Acute Phase | First 6–72 hours | Dramatic improvement | Therapeutic Hypothermia (TH) | ↓ Mortality, ↓ Severe Disability |
| Chronic Phase | 72 hours to death | Minimal progress | Traditional rehab, assistive tech | Marginal gains over decades |
Acute Phase: A Revolution in Neonatal Neuroprotection
What Changed:
- Therapeutic Hypothermia (TH): Cooling infants to ~33.5°C within 6 hours of birth for 72 hours.
- Adoption Timeline: Became standard of care around 2010.
- Clinical Impact:
- 25% relative reduction in death or major neurodevelopmental disability.
- Improved motor and cognitive outcomes at 18–24 months.
- First and only proven neuroprotective therapy for severe hypoxic-ischemic encephalopathy (HIE).
Why It Matters:
- In a field where 5% improvement is considered meaningful, 25% is seismic.
- TH shifted the trajectory of care from reactive to proactive.
Chronic Phase: The Long Plateau
The Harsh Reality:
- After the 72-hour window, families enter a world of limited innovation.
- Most treatments—PT, OT, speech therapy—have remained fundamentally unchanged for decades.
- Assistive technologies have improved, but they support adaptation, not recovery.
What Hasn’t Improved:
- Neuroregeneration therapies: Still experimental, not widely available.
- Pharmacological Options: Few targeted drugs for neuroregeneration or plasticity.
- Outcome metrics: Long-term independence, mobility, and cognition remain stubbornly static.
Supporting Evidence
1. Lack of Breakthroughs in CP Rehabilitation
Recent clinical trials cataloged by The United Cerebral Palsy Foundation show that while numerous studies are exploring therapies across the lifespan, few have demonstrated transformative improvements in motor function or cognitive outcomes during the chronic phase. Most interventions offer incremental gains, such as improved mobility or reduced spasticity, but do not reverse or significantly alter the neurological trajectory.
2. Clinical Trials Focused on Symptom Management
According to Cerebral Palsy Guide, many ongoing trials aim to refine existing therapies—like physical therapy, assistive devices, and pharmacological interventions—but none have shown consistent, long-term efficacy in changing the course of CP once established. The trials often report short-term functional improvements without sustained gains in independence or quality of life.
- A 2023 randomized clinical trail found that even individually tailored home-based interventions in chronic TBI improved generic quality of life—but not outcomes or social participation.
- A 2024 book titled “Traumatic Brain Injury” states that long-term neurorehabilitation shows promise but is limited by access, funding, and systemic fragmentation.
3. Insurers Commonly Cite Studies to Deny Long-Term PT in CP and Brain Injury
- In Smith v. Aetna Life Insurance Company (2017), Aetna’s internal expert witness presented Novak et al. (2013) as evidence that routine PT for CP lacks the precision and repetition needed for lasting neuroplastic change. Download the PDF: Develop Med Child Neuro – 2013 – Novak – A systematic review of interventions for children with cerebral palsy
- In Doe v. UnitedHealthCare Services, Inc. (2014), United successfully argued that the EBRSR and Winstein et al. (2016) guidelines showed no industry-accepted basis for long-term PT in chronic stroke.
Our Personal Treatment Journey from November 2000 through 2025
My daughter Alissa, was born in November 2000 with severe hypoxic-ischemic encephalopathy (HIE). At that time, Therapeutic Hypothermia (TH) was still 10 years from widespread use. The standard of care in 2000 was based on:
- Stabilization: Focused on maintaining oxygenation, ventilation, and perfusion.
- Seizure management: Anticonvulsants like phenobarbital were used if seizures occurred.
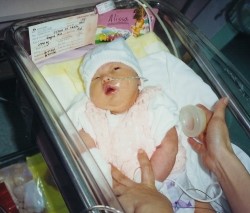
Alissa Nov. 2000 in the NICU
I remember the setting of the NICU like it was yesterday. A small heat lamp was placed over Alissa’s enclosed bed. They gave her a small knitted cap to keep her head even warmer. I remember the heat, the cap, the monitor wires. Alissa was given prophylactic phenobarbital, which put her into a catatonic state to prevent seizures. Looking back and knowing what we know now, the heat and the phenobarbital were mistakes. Modern treatment would cool the body or at least the brain and advanced EEG would be used to monitor for seizures in advance and risky anti-seizure meds would only be given if needed.
Ironically, even though cooling was still 10 years away from widespread use, we did have the internet in 2000 and about 1 week after birth I stumbled across a study for brain cooling after HIE. I spoke with Alissa’s NICU doctor about the study. Amazingly he had also heard about the study, but he dismissed it because without the proper equipment, brain cooling can be risky. We would have literally needed to pack Alissa’s head in ice and in her extremely medically vulnerable state that would have been very dangerous.
That was the first time I felt the pain of regret with Alissa. It would not be the last.
A survey of treatments available in the year 2000 vs 2025
Surprisingly, with the exception virtual reality all the current mainstream treatment methods for CP already existed in some form in the year 2000. A quick survey of modern mainstream treatments include physiotherapy techniques, botulinum toxin injections, selective dorsal rhizotomy, intrathecal baclofen, constraint-induced movement therapy, robotic-assisted training, biofeedback. and novel rehabilitation technologies like virtual reality.
Of this list, only virtual reality was not available in the year 2000.
Physiotherapy: Key concepts developed in 1940s and only incremental progress
Physiotherapy for children with cerebral palsy (CP) traces its structured origins to the 1940s–50s, with Berta and Karel Bobath’s development of Neurodevelopmental Treatment (NDT) in the UK. Around the same time, in 1955, Glen Doman co-founded the Institutes for the Achievement of Human Potential (IAHP) in Philadelphia, pioneering a method that emphasized motor patterning, sensory stimulation, and intensive, goal-directed therapy.
Ironically, what’s now considered cutting-edge in mainstream physiotherapy—comprehensive, goal-directed rehabilitation with high therapy dosage—mirrors the principles Doman championed over 70 years ago. Yet, despite this convergence, a longstanding and often bitter divide persists between IAHP and major medical institutions such as the AAP, AACPDM, NIH, and organizations like United Cerebral Palsy.
Critics have long dismissed Doman’s work due to its private, for-profit model and reliance on anecdotal evidence. However, rigorous peer-reviewed studies have consistently shown that traditional physiotherapy yields limited outcomes. Only recently, as mainstream approaches began adopting Doman’s intensive, goal-driven framework, have measurable improvements emerged.
The encouraging news is that Cerebral Palsy Treatments in 2025 are finally achieving meaningful—if still modest—progress. But it’s hard to ignore that it took the mainstream nearly eight decades to embrace what Boboth & Doman understood in the 1950s.
Botox injections, selective dorsal rhizotomy, & intrathecal baclofen
Botox injections, selective dorsal rhizotomy, & intrathecal baclofen were widely available in 2000. No significant advancements has been made in their deployment methods.
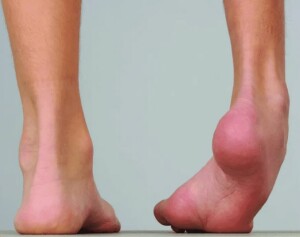
Cerebral Palsy-Drop Foot
When Alissa was 19 months old, we tried Botox injections to help her stand and eventually walk. Although she was eager, her tight heel cords and weak ankles made independent standing impossible. In a supported stance, her feet rolled inward severely.
Therapists and orthopedists proposed using Botox to relax the rigid muscles causing toe pointing, followed by serial casting to stretch the heel cords. The goal was to get her standing during the Botox window, allowing proprioceptive signals to help the brain form new neural pathways. The hope was that as the Botox wore off, muscle rigidity would lessen and functional movement would improve.
While this approach is grounded in solid science, it had drawbacks. From a Dynamic Systems Theory(DST) perspective, Botox and casting introduced new variables and weakened her muscles, making it harder for new movement patterns to override existing ones.
Ultimately, the intervention didn’t yield lasting functional gains. Although her heel cords improved and the drop foot was resolved, one foot was over-corrected during casting—leading to arch collapse and excessive ankle rolling. The casting process relied on manual positioning within a brief 1–2 minute window before the resin hardened, and unfortunately, the correction went too far, causing permanent deformity.
We considered corrective surgery, but given the underlying brain injury driving her muscle abnormalities, we felt the risks outweighed the potential short-term benefits. Without addressing the root neurological cause, the original issues would likely return.
A brief but important aside: a true breakthrough in Alissa’s journey wasn’t Botox or Baclofen—quick fixes that generate same-day revenue in the doctors office—but the fortunate addition of Esther Thelen to BRIGHT’s Scientific Advisory Board. A pioneering developmental psychologist, Thelen revolutionized how researchers understand infant motor and cognitive development through Dynamic Systems Theory. Though she passed in 2004, and much of her work faded from focus, I believe her framework remains vital to shaping truly transformative approaches to brain injury rehabilitation in the near future.
Botulinum Toxin: Short-Term Relief, No Sustained Gains
- Study: Botulinum toxin A treatment in children with cerebral palsy: a systematic review
- Journal: Developmental Medicine & Child Neurology, 2021
- Findings: Botox injections showed short-term improvements in spasticity, but no consistent long-term functional benefits. Repeated injections were needed, and effects often plateaued or diminished over time.
Intrathecal Baclofen: Modest Motor Gains, Significant Risks
- Study: Intrathecal baclofen efficacy for managing motor function and spasticity severity in patients with cerebral palsy: a systematic review and meta-analysis
- Journal: BMC Neurology, 2024
- Findings: While intrathecal baclofen significantly reduced spasticity (Ashworth scale), motor function improvement was minimal—only a 9.6% increase in GMFM scores. Moreover, complication rates were high, including infections, seizures, and cerebrospinal fluid leaks.
- https://bmcneurol.biomedcentral.com/articles/10.1186/s12883-024-03647-7
Long-Term Baclofen Use: Functional Decline Despite Spasticity Control
- Study: Long term effect (more than five years) of intrathecal baclofen on impairment, disability, and quality of life in patients with severe spasticity
- Journal: Journal of Neurology, Neurosurgery & Psychiatry, 2004 (still widely cited)
- Findings: Although spasticity improved, disability and perceived health status worsened over time. This suggests that baclofen may reduce tone but doesn’t translate into meaningful functional gains.
- https://jnnp.bmj.com/content/75/11/1553
Ed Taub, Mike Merzenich and the Fringe Science of Neuroplasticity
By early 2002, I had assembled BRIGHT’s Scientific Advisory Board, intentionally recruiting a diverse mix of engineers, clinicians, psychologists, and other innovative thinkers. Some doctors and neurologists dismissed their contributions as outside their domain. Ed Taub, notably involved in one of the most controversial episodes in U.S. scientific history, was among them. Yet his work was groundbreaking—and is now widely recognized as a model for effective modern treatment. BRIGHT saw its value clearly, even back in 2002. Again, another case of mainstream practice taking decades to catch-up.
Ed Taub faced resistance because his early work used animal models, but also because his core scientific ideas challenged entrenched beliefs in neuroscience and rehabilitation medicine. Taub and Merzenich faced no resistance at BRIGHT and although neither were able to clinically treat Alissa, we adapted their theories into Alissa’s personalized therapy program.
Resistance to Taub’s Theories
Taub’s central concept of “learned non-use”—the idea that patients stop using impaired limbs not because they physically can’t, but because they’ve adapted behaviorally—was radically counterintuitive at the time.
- Traditional view: Paralysis or motor deficits were seen as purely neurological and irreversible.
- Taub’s view: Behavioral conditioning and targeted therapy could “unlock” dormant motor abilities, even years after injury.
This flew in the face of decades of clinical dogma. Many scientists and clinicians were skeptical, especially because:
- His early work was based on animal models, which were controversial even before the Silver Spring Monkeys case.
- He wasn’t a medical doctor, but a psychologist, which made some neurologists dismiss his work as outside their domain.
- Constraint Induced (CI) therapy required intensive, non-standard protocols—like restraining the unaffected limb—which seemed extreme or impractical to many therapists.
Pushback on Neuroplasticity
Taub’s work was among the first to show that neuroplasticity—the brain’s ability to reorganize itself—could be harnessed therapeutically. But in the 1980s and early 1990s, neuroplasticity was still considered fringe science.
- Many researchers believed the adult brain was largely “fixed” after development.
- Taub’s findings suggested that functional recovery was possible even years after stroke or injury, which contradicted prevailing rehabilitation timelines.
It wasn’t until other scientists like Michael Merzenich and Norman Doidge began publishing complementary findings that Taub’s ideas gained traction.
Institutional Barriers
Even after CI therapy showed success in trials:
- Insurance companies were slow to cover it, citing lack of standardization.
- Hospitals hesitated to adopt it due to the need for specialized training and longer therapy sessions.
- The Veterans Administration recognized it as a preferred treatment for TBI, but lacked therapists trained in the method
Redemption Through Results
Despite the resistance, Taub’s persistence paid off:
- CI therapy became the first stroke rehab method to succeed in a multi-center randomized clinical trial funded by the NIH
- His work was named one of the top 10 translational neuroscience accomplishments of the 20th century
Taub’s struggle wasn’t just about ethics. It was about challenging the scientific status quo, and ultimately proving that behavioral neuroscience could revolutionize rehabilitation.
I’m deeply grateful for the years of work by Taub and Merzenich to challenge outdated scientific norms. But the truth is, because of their involvement with BRIGHT, Alissa was already receiving an optimized neuroplasticity-based treatment program in 2002. Therefore, her program then is virtually identical to the modern approaches used today. And while neuroplasticity-based treatment like CI is sound, the truth is that it is still not enough to produce radical changes in long term outcomes for someone like Alissa.
https://brainsciencepodcast.com/bsp/119-taub1
https://www.uab.edu/cas/psychology/people/emeritus-faculty/edward-taub